The temporary technical problem in the data network connections
A temporary technical problem occurred in the data network connections of Docrates Cancer Center. We apologise for any delays caused...
Read moreMon–Fri 8–16
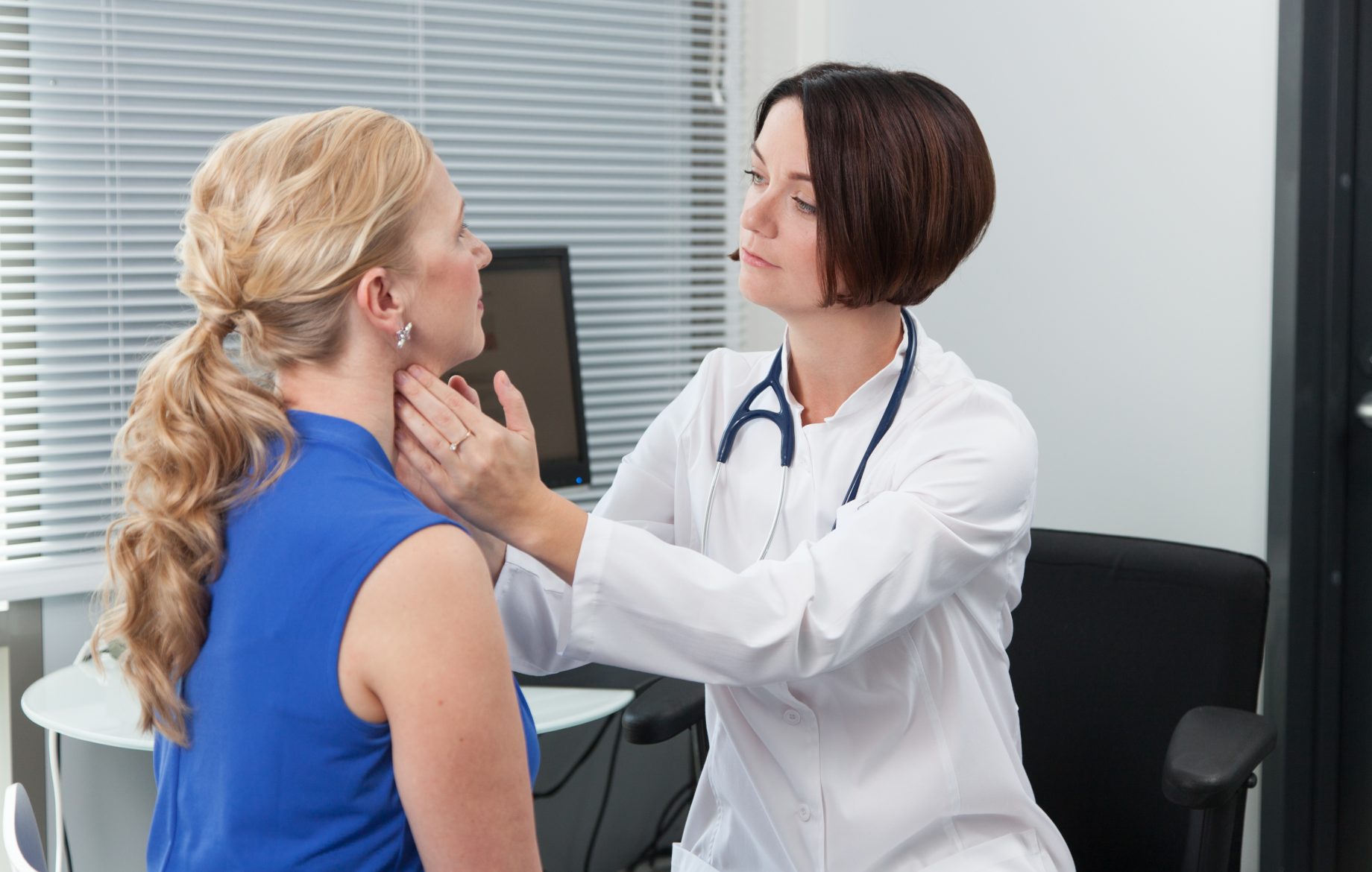
Thyroid cancer has increased in recent years. It is known to be more common in women than in men. On average, thyroid cancer is diagnosed in patients 25 to 65 years of age.
It is reassuring to know that thyroid cancer is treatable in most cases. Thyroid cancer has one of the highest five-year survival rates of all cancers. This means that thyroid cancer patients have a very good chance of being cancer-free five years from the diagnosis.
There are three types of thyroid cancers: papillary, follicular and medullary thyroid cancer. They are distinguished from each other on the basis of the microscopic cytological picture, and they behave differently. Papillary thyroid cancer is the most common type of thyroid cancer and, fortunately, also the least malignant. Follicular thyroid cancer is the second most common, and the medullary type is the least common.
In most cases, the cause of thyroid cancer cannot be identified. The only known risk factor for thyroid cancer is exposure to ionising radiation, such as radiotherapy administered to the neck area years ago or exposure to a nuclear disaster. Such causes are extremely rare. Treatment of hyperthyroidism with radioiodine does not increase the risk of cancer. After the emission of radioactive iodine into the air during the Chernobyl nuclear plant disaster, a significant increase in the occurrence of thyroid cancer was detected in nearby regions.
The most common and often only symptom of thyroid cancer is a lump in the neck, growing quite slowly over months. Such a palpable lump detected in the neck must always be examined. Thyroid cancer may also cause swelling of lymph nodes in the neck. If the cancer has spread into the structures of the neck, this may cause hoarseness or difficulty swallowing. However, these can also be general symptoms of other diseases.
A lump in the thyroid gland can be examined by ultrasound scans and thin-needle biopsies. An ultrasound scan does not tell whether a tumor is malignant or benign, but it may give some information about its nature and helps to target a thin sampling needle accurately to the tumor. The cells remaining in the needle are analysed under a microscope. This can only be done by a pathologist.
A thin-needle biopsy is usually a reliable method for detecting papillary and medullary thyroid cancers, whereas the diagnosis of follicular cancer usually requires an additional, larger biopsy specimen of the thyroid gland. Often the lobe of the thyroid gland in which the tumor resided is removed at the same time.
The most reliable way of determining the nature of a lump is to remove it. This is recommended if the lump is large, exceptionally hard and rapidly grown, or if the patient has previously received radiotherapy to the neck area. Lab tests are usually not useful for the diagnosis of thyroid cancer.
Treatments for thyroid cancer include surgery, radioiodine therapy, external radiotherapy and chemotherapy. Surgery is the basic treatment for thyroid cancer. The objective is to remove the entire thyroid gland as thoroughly as possible. Possibly affected nearby lymph nodes are removed at the same time. In papillary and follicular cancers, radioiodine therapy is administered postoperatively. Patients operated on will need a thyroxine supplement for the rest of their life; after the removal of the thyroid gland, the body no longer produces this hormone.
A temporary technical problem occurred in the data network connections of Docrates Cancer Center. We apologise for any delays caused...
Read more
Hannu Nurmio was aware that prostate cancer is the most common cancer in older men. However, after the diagnosis was confirmed,...

Early detection of colorectal cancer is crucial for successful treatment. If diagnosed early, up to 90% of cancers can be...

Docrates Cancer Center is the first service provider in the Nordic region to launch a new experimental alpha radiation treatment...
Contact us!
Mon-Thu 8:00-18:00, Fri 8:00-16:00
